Role of mental health evaluations in trauma healing 2026
Many people believe mental health evaluations exist solely to diagnose disorders and assign labels. This misconception prevents trauma survivors from accessing one of the most powerful tools for personalized healing. Mental health evaluations actually create detailed roadmaps for recovery, especially for those dealing with PTSD, anxiety, and relationship challenges. Through trauma-informed assessments, therapists uncover the specific ways past experiences shape current struggles and design targeted treatment plans. When paired with evidence-based approaches like EMDR therapy, these evaluations transform healing from guesswork into precision care. Understanding how evaluations work empowers you to take control of your recovery journey in California.
Table of Contents
Key takeaways
| Point | Details |
|---|---|
| Evaluations reveal personalized trauma impacts | Assessments identify how specific experiences affect your mental health and relationships today |
| They guide effective EMDR treatment plans | Evaluations help therapists target the right memories and develop safe, customized healing strategies |
| Trauma-informed approaches improve outcomes | Sensitive assessments designed for trauma survivors lead to more accurate understanding and respectful care |
| Ongoing evaluations track healing progress | Regular assessments measure symptom changes and help adjust therapy for continued growth |
Understanding mental health evaluations for trauma
Mental health evaluations serve as comprehensive assessments that examine your emotional, psychological, and behavioral patterns to create effective treatment strategies. For trauma survivors, these evaluations go beyond surface symptoms to explore how past experiences continue influencing present-day functioning. Trauma assessments identify underlying factors essential for treatment planning, making them foundational to successful therapy outcomes.
A trauma-informed mental health evaluation typically includes several key components. Therapists gather detailed personal history, including childhood experiences, significant life events, and previous trauma exposure. They assess current symptoms like intrusive thoughts, hypervigilance, emotional numbness, or relationship difficulties. Clinical interviews explore how trauma affects daily life, work performance, and interpersonal connections. Standardized questionnaires measure symptom severity and track specific challenges related to PTSD, anxiety, or depression.
The evaluation process follows a structured yet flexible approach. Your first session involves building rapport and explaining the assessment purpose in a safe, non-judgmental environment. Therapists ask open-ended questions about your experiences, allowing you to share at your own pace without pressure. They observe behavioral cues, emotional responses, and communication patterns that reveal trauma's impact. You might complete written assessments between sessions to provide additional insight into your mental health status.
Why are these evaluations crucial before starting therapy? They prevent misdiagnosis by distinguishing between similar conditions like depression and complex PTSD. Evaluations identify co-occurring issues that require simultaneous attention, such as anxiety disorders alongside trauma symptoms. They establish baseline measurements for tracking progress throughout treatment. Most importantly, evaluations ensure therapy approaches match your specific needs rather than applying generic protocols.
Trauma-informed evaluations uncover how PTSD manifests in your unique situation. Some survivors experience primarily emotional symptoms like shame or guilt. Others struggle with physical manifestations including chronic pain or sleep disturbances. Relationship impacts vary widely, from attachment difficulties to communication breakdowns. Understanding these specific patterns allows therapists to design interventions addressing your actual challenges rather than assumed symptoms.
The role of mental health evaluations in EMDR therapy and healing from trauma
EMDR therapy relies heavily on thorough mental health evaluations to maximize effectiveness and safety. Personalized treatment plans enhance EMDR therapy outcomes by identifying which traumatic memories require processing first. Evaluations reveal the connections between past trauma and current symptoms, creating a clear treatment roadmap. Without this foundation, EMDR sessions might target less critical memories or miss important trauma networks.
Mental health evaluations help establish specific, measurable therapy goals aligned with your healing priorities. You might want to reduce nightmares, improve relationship communication, or manage anxiety in social situations. Evaluations clarify which symptoms stem directly from trauma versus other mental health conditions. This distinction matters because EMDR specifically targets trauma-based issues, while other therapeutic approaches might better address different concerns. Clear goals keep therapy focused and allow you to recognize progress as it happens.
The evaluation process guides selection of trauma targets in EMDR sessions. Therapists identify which memories contribute most significantly to current distress. They map out how different traumatic events connect to form larger trauma networks requiring systematic processing. Evaluations also assess your readiness for trauma processing by examining coping skills, support systems, and emotional regulation capacity. Starting EMDR without adequate preparation can feel overwhelming and potentially retraumatizing.
For anxiety and relationship healing, trauma-informed assessments reveal how past experiences created current patterns. Childhood trauma often establishes attachment styles affecting adult relationships. Evaluations uncover these connections, allowing EMDR to target the root experiences rather than just managing symptoms. When therapists understand how trauma shaped your worldview, they can help you process memories that maintain anxiety, avoidance, or relationship conflicts.
Benefits of comprehensive evaluations before EMDR include:
Identifying stabilization needs before trauma processing begins
Recognizing triggers that might arise during therapy sessions
Establishing safety protocols for managing intense emotions
Creating realistic timelines based on trauma complexity
Determining whether additional support services would enhance outcomes
Pro Tip: Share your complete history during evaluations, even details that seem unrelated or embarrassing. Therapists need the full picture to design effective EMDR treatment. Information you withhold might be the key to understanding persistent symptoms or treatment resistance.
Evaluations also help therapists gauge your capacity for bilateral stimulation, the core mechanism in EMDR. Some individuals find eye movements distracting or uncomfortable due to specific trauma histories. Knowing this beforehand allows therapists to use alternative forms like tactile tapping or auditory tones. This personalization ensures EMDR remains accessible and effective regardless of individual differences.
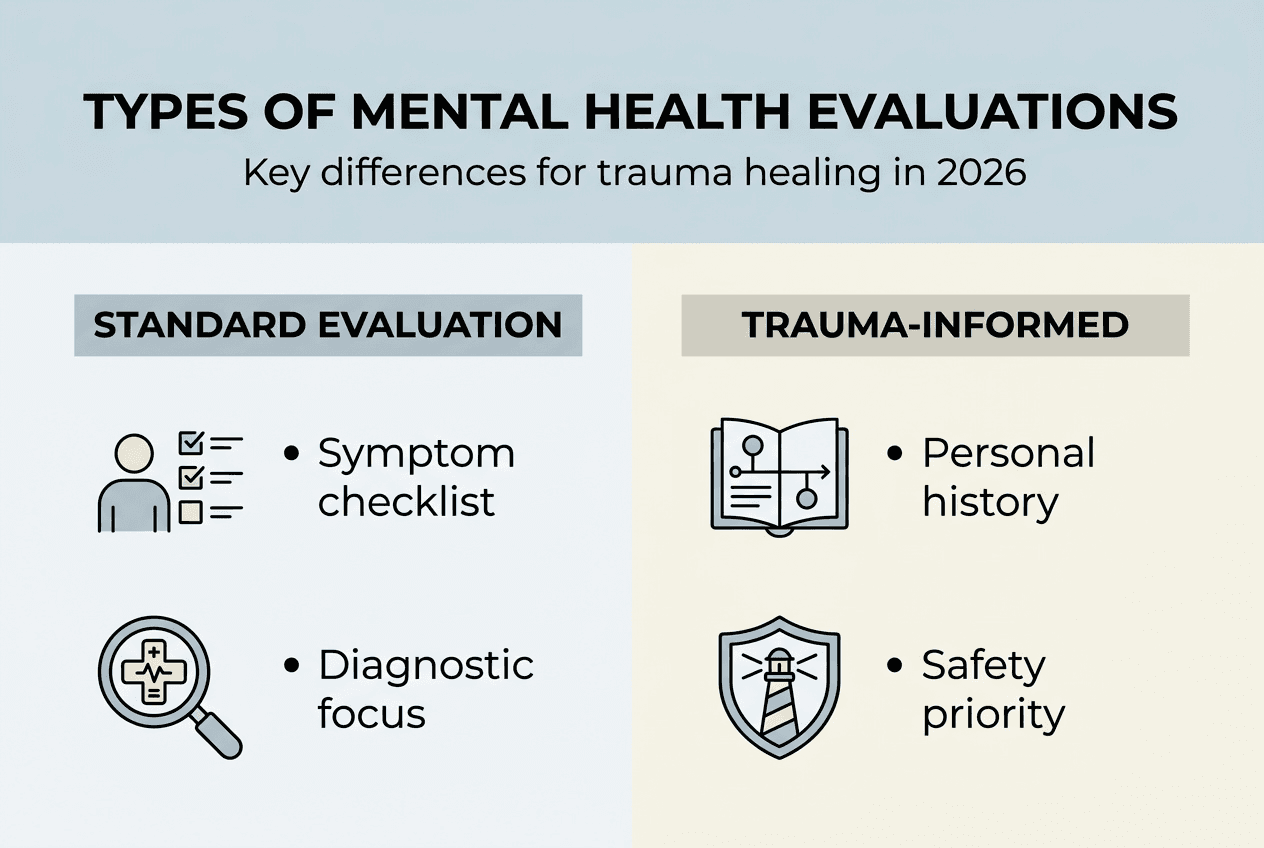
Comparing trauma-informed mental health evaluations with standard evaluations
Trauma-informed evaluations differ fundamentally from standard mental health assessments in approach, sensitivity, and outcomes. Trauma-informed assessments incorporate sensitivity to complex trauma impacts that standard evaluations might overlook or misinterpret. Understanding these differences helps you choose the right evaluation type for your healing needs.
Standard mental health evaluations typically follow diagnostic criteria from the DSM-5, focusing on symptom checklists and disorder identification. They work well for straightforward conditions like generalized anxiety or major depression. However, they often miss the nuanced ways trauma affects mental health, particularly when symptoms don't fit neatly into diagnostic categories. Standard evaluations might label complex trauma responses as personality disorders or treatment-resistant depression.
Trauma-informed evaluations recognize that behaviors serving as survival mechanisms during trauma might appear dysfunctional in current contexts. They explore the adaptive purpose of symptoms rather than simply cataloging problems. This perspective shift prevents pathologizing normal trauma responses and builds a foundation for compassionate, effective treatment.
| Aspect | Standard Evaluation | Trauma-Informed Evaluation |
|---|---|---|
| Primary Focus | Symptom identification and diagnosis | Understanding trauma's impact on functioning |
| Question Style | Direct, checklist-based queries | Open-ended, narrative exploration |
| Clinician Approach | Neutral, diagnostic stance | Collaborative, empowering partnership |
| Treatment Goals | Symptom reduction | Healing trauma roots and building resilience |
| Cultural Sensitivity | Variable, often limited | Central to assessment process |
Choosing the right evaluation involves several important steps:
Research therapists' training in trauma-specific assessment methods and certifications in trauma-focused therapies like EMDR.
Ask potential providers how they approach trauma history during evaluations and whether they use trauma-informed frameworks.
Inquire about assessment tools specifically designed for trauma survivors rather than generic mental health questionnaires.
Discuss your concerns about safety, pacing, and emotional regulation during the evaluation process itself.
Verify that evaluations include assessment of strengths, resources, and resilience factors alongside challenges.
Trauma-informed evaluations lead to more accurate diagnoses because they account for how trauma symptoms mimic other conditions. Complex PTSD can look like borderline personality disorder. Dissociation might be mistaken for attention deficits. Hypervigilance resembles generalized anxiety. Trauma-informed assessors recognize these overlaps and investigate thoroughly before concluding diagnoses.
Respect forms another crucial difference. Trauma survivors often experienced violations of boundaries, autonomy, or dignity. Standard evaluations might inadvertently recreate these dynamics through intrusive questions or power imbalances. Trauma-informed evaluations prioritize your agency, allowing you to control disclosure pace and content. Therapists explain the purpose behind questions and respect your right to decline answering without judgment.
These evaluations also prepare clients for effective treatment by establishing safety and trust from the first interaction. When you feel respected and understood during assessment, you're more likely to engage authentically in subsequent therapy. This foundation proves especially valuable for EMDR and other trauma-focused interventions requiring vulnerability and emotional processing.
How mental health evaluations support ongoing healing and relationship growth
Mental health evaluations function as ongoing tools throughout your healing journey, not just one-time diagnostic events. Routine evaluations help track trauma recovery and refine treatments for sustained progress. Regular assessments measure how therapy impacts your daily life, relationships, and overall wellbeing. They provide objective data showing improvement even when progress feels slow or invisible.
Evaluations serve as therapy milestones, marking transitions between treatment phases. After completing initial EMDR processing of core trauma memories, reassessment determines whether additional targets require attention. When anxiety symptoms decrease significantly, evaluations help shift focus toward relationship healing or personal growth goals. These checkpoints prevent therapy from continuing unnecessarily or ending prematurely.
Tracking symptom changes over time reveals patterns that might otherwise go unnoticed. You might not realize how much your sleep improved or how rarely panic attacks occur compared to six months ago. Standardized measures provide concrete evidence of healing, which builds motivation during difficult therapy phases. Evaluations also identify emerging issues early, allowing prompt intervention before they escalate.
For relationship growth, periodic evaluations assess how trauma healing translates into interpersonal improvements. They measure attachment security, communication effectiveness, conflict resolution skills, and emotional intimacy. Partners sometimes participate in evaluations to provide their perspective on relationship changes. This comprehensive view ensures therapy addresses real-world functioning, not just internal symptom reduction.
Benefits of ongoing mental health evaluations include:
Validating progress through measurable improvements in standardized assessments
Identifying when treatment approaches need modification based on changing needs
Preventing relapse by catching early warning signs of symptom return
Documenting healing for insurance, legal, or personal records
Maintaining therapeutic alignment between your goals and actual treatment focus
| Evaluation Metric | Initial Assessment | 3-Month Follow-Up | 6-Month Follow-Up | | --- | --- | --- | | PTSD Symptom Severity | Severe (Score 68) | Moderate (Score 42) | Mild (Score 24) | | Anxiety Level | High (Score 18) | Moderate (Score 12) | Low (Score 6) | | Relationship Satisfaction | Low (Score 3/10) | Moderate (Score 6/10) | High (Score 8/10) | | Sleep Quality | Poor (4 hrs/night) | Fair (6 hrs/night) | Good (7 hrs/night) |
Pro Tip: Keep a journal between evaluation sessions tracking symptoms, triggers, coping successes, and relationship moments. This record provides accurate information during assessments rather than relying on memory alone. Specific examples help therapists understand your actual progress and remaining challenges.
Ongoing evaluations support renewed goal setting as you heal. Early therapy might focus on safety and stabilization. Mid-treatment goals often involve trauma processing and symptom reduction. Later stages emphasize post-traumatic growth, meaning development, and thriving beyond survival. Regular assessments ensure your therapy evolves with your changing needs rather than following a rigid protocol.
These evaluations also normalize the non-linear nature of trauma recovery. Healing rarely progresses in straight lines. You might experience setbacks, plateaus, or sudden breakthroughs. Regular assessments contextualize these fluctuations, distinguishing temporary struggles from genuine treatment ineffectiveness. This perspective prevents discouragement and supports persistence through challenging phases.
Support your trauma healing journey with expert care
Navigating trauma recovery becomes more manageable with professional support designed specifically for your needs. Alvarado Therapy specializes in trauma-informed mental health evaluations that honor your experiences while creating clear pathways toward healing. Our licensed therapists understand how PTSD, anxiety, and relationship challenges intersect, offering comprehensive assessments that inform personalized treatment plans.
Whether you're considering online EMDR trauma therapy or exploring in-person options across California, our team provides culturally responsive care in English and Spanish. We offer therapy consultations to discuss your specific situation and determine the most effective approach for your healing goals. Our PTSD and complex trauma services integrate evidence-based methods with compassionate support, creating a safe space for transformation. Taking the first step toward evaluation opens doors to understanding yourself more deeply and building the life you deserve.
Frequently asked questions
What is a mental health evaluation?
A mental health evaluation is a comprehensive assessment examining your emotional, psychological, and behavioral health to guide treatment decisions. It involves clinical interviews, standardized questionnaires, and observation to understand your symptoms, history, and functioning. The evaluation identifies diagnoses, uncovers underlying issues, and creates personalized care plans addressing your specific needs.
How do trauma-informed mental health evaluations differ from standard evaluations?
Trauma-informed evaluations focus specifically on understanding how past trauma affects current mental health with sensitivity to re-traumatization risks. They use open-ended questions, collaborative approaches, and strength-based perspectives rather than just diagnostic checklists. Standard evaluations follow broader protocols that might miss complex trauma manifestations or inadvertently recreate harmful power dynamics.
Why are mental health evaluations important before starting EMDR therapy?
Evaluations identify which traumatic memories require processing and establish personalized therapy goals for effective EMDR treatment. They assess your readiness for trauma work by examining coping skills, support systems, and emotional regulation capacity. Understanding your complete trauma history ensures therapy targets root causes safely rather than overwhelming you with premature processing.
How often should mental health evaluations be done during therapy?
Evaluations typically occur at intake, every three to six months during active treatment, and at significant therapy milestones or transitions. Frequency depends on your individual progress, treatment complexity, and specific goals requiring ongoing measurement. More frequent assessments might be necessary if symptoms fluctuate significantly or treatment approaches need adjustment based on emerging issues.