Step-by-step trauma healing: EMDR guide for Californians
You've tried to move forward. Maybe you've journaled, talked to friends, or told yourself time heals everything. But the memories still surface, your body still tenses, and the weight of what happened hasn't lifted. That feeling of being stuck despite wanting to heal is one of the most common experiences among adults recovering from trauma. The good news is that evidence-based therapies like EMDR (Eye Movement Desensitization and Reprocessing) and trauma-informed counseling offer a structured, proven path forward. This guide walks you through that path, step by step, so you can move from surviving to genuinely healing.
Table of Contents
Key Takeaways
| Point | Details |
|---|---|
| Safety comes first | Before any trauma work, building safety and support is essential for true progress. |
| Stepwise healing works | Following clear, evidence-based steps leads to reliable improvement in PTSD and trauma symptoms. |
| EMDR matches CBT | Research shows EMDR is as effective as trauma-focused CBT for most PTSD symptoms. |
| Track your progress | Use personal milestones and symptom changes to measure healing and adjust your plan. |
Understanding trauma and the healing process
Trauma is not just a bad memory. It's a disruption in how your brain and body process experience. When something overwhelming happens and your system can't fully integrate it, the memory gets stored in a fragmented, emotionally raw way. That's why a smell, a sound, or a certain look from someone can trigger a flood of feelings that seem out of proportion to the moment.
Common trauma symptoms include:
Emotional: Anxiety, shame, emotional numbness, irritability, or sudden sadness
Psychological: Intrusive memories, nightmares, hypervigilance, difficulty concentrating
Physical: Tension, fatigue, sleep disruption, chronic pain without clear medical cause
Among California adults, two of the most frequently treated trauma types are PTSD (Post-Traumatic Stress Disorder) and childhood or developmental trauma. PTSD often follows a single identifiable event, like an accident or assault. Childhood trauma tends to be more layered, shaped by repeated experiences of neglect, abuse, or instability during formative years.
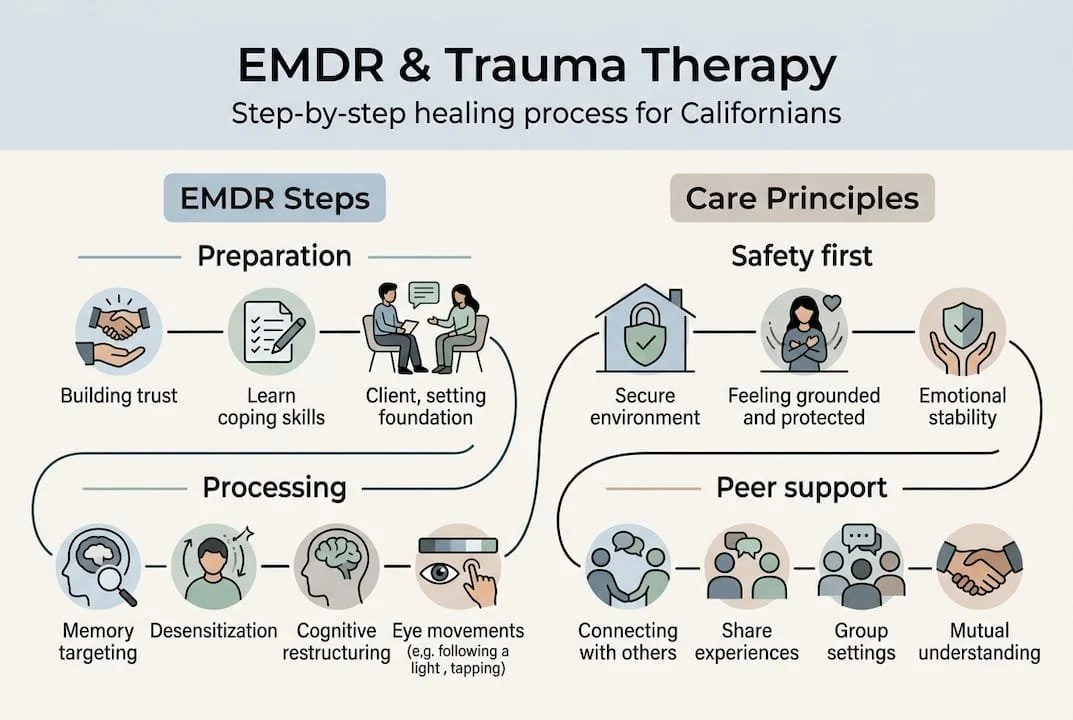
The two primary treatment approaches covered in this guide are EMDR and trauma-informed therapy. EMDR uses bilateral stimulation (often eye movements) to help your brain reprocess stuck memories. Trauma-informed therapy is a broader framework that shapes how any therapy is delivered, prioritizing your sense of safety and control throughout.
A step-by-step approach works because trauma healing isn't linear, but it does have identifiable stages. Moving through them with intention reduces overwhelm and builds momentum. The trauma recovery workflow used in trauma-informed practice reflects this sequenced structure.
According to SAMHSA, trauma-informed care principles include safety, trustworthiness, peer support, collaboration, and empowerment. These aren't just values. They are the operating conditions that make healing possible. When your therapy environment reflects these principles, your nervous system can finally start to settle.
Pro Tip: When researching therapists, ask directly how they incorporate trauma-informed principles into their work. A good therapist will welcome that question.
For a deeper look at how these stages connect, the guide on lasting trauma healing offers a useful companion framework.
Preparing for trauma healing: Setting a safe foundation
Before you begin processing traumatic memories, you need a stable base. Jumping into deep trauma work without preparation can actually increase distress. Think of it like building a house: the foundation has to come first.
Here's a numbered checklist to help you assess readiness:
Physical safety: Are you currently safe from harm, abuse, or crisis?
Support system: Do you have at least one trusted person you can reach out to after hard sessions?
Therapist selection: Have you found a licensed, trauma-informed therapist who uses EMDR or a comparable evidence-based method?
Consent and clarity: Do you understand what therapy will involve and feel comfortable asking questions?
Coping tools: Do you have at least two or three grounding strategies you can use when emotions spike?
The starting trauma therapy checklist can help you work through each of these areas before your first session.
Here's a quick comparison of what prepared versus unprepared entry into trauma therapy can look like:
| Factor | Prepared | Unprepared |
|---|---|---|
| Safety | Stable living situation | Ongoing unsafe environment |
| Support | At least one trusted contact | Isolated, no support network |
| Coping skills | 2 to 3 grounding techniques ready | No tools for emotional regulation |
| Therapist fit | Trauma-informed, EMDR-trained | General counselor, no trauma focus |
| Expectations | Realistic, flexible | Expecting quick or linear results |
Tools that help during this stage include a journal for tracking triggers, a written list of your known stress responses, and a clear agreement with your therapist about session pacing.
Important: If you are currently experiencing thoughts of self-harm, active abuse, or a mental health crisis, please contact the 988 Suicide and Crisis Lifeline by calling or texting 988 before beginning trauma therapy. Safety always comes first.
The trauma-informed principles of safety and empowerment apply here too. You should never feel pressured to move faster than you're ready to. A good therapist will follow your lead.
Step-by-step trauma healing: EMDR and therapy workflows
Once your foundation is in place, you move into the active healing stages. Here's how the process typically unfolds:
Stabilization: Build emotional regulation skills. Learn grounding techniques like deep breathing, the 5-4-3-2-1 sensory method, and safe-place visualization.
History and assessment: Work with your therapist to map out your trauma history, identify target memories, and set treatment goals.
EMDR preparation: Your therapist introduces bilateral stimulation and ensures you feel comfortable with the process before targeting any memories.
Desensitization: The core EMDR phase. You hold a traumatic memory in mind while following the therapist's guided eye movements or taps. The memory gradually loses its emotional charge.
Installation: Positive beliefs replace the negative ones linked to the trauma (for example, shifting from "I am powerless" to "I handled it and I'm safe now").
Body scan: You check for any remaining physical tension connected to the memory.
Closure and integration: Each session ends with grounding. Between sessions, you process what surfaced and build on your gains.
For a detailed breakdown of each phase, the EMDR therapy steps guide walks through what to expect in real sessions.
The APA's 2025 PTSD guidelines include a conditional recommendation for EMDR in adults with PTSD, reflecting its strong evidence base. Research shows EMDR recovery rates of approximately 43.6% in NHS service settings, with reliable improvement seen in 60 to 80% of participants across broader studies.
Pro Tip: After an EMDR session, plan for a low-demand evening. Avoid scheduling high-stress commitments right after. Your brain is still processing, and rest supports integration.
For California-specific context on accessing this care, EMDR for trauma in California covers both effectiveness and how to find qualified providers.
Troubleshooting and overcoming common challenges
Stalling in trauma therapy doesn't mean you're failing. It usually means your nervous system needs more time, more safety, or a slightly different approach. Setbacks are a normal part of the process, not a sign that healing isn't possible.
Common challenges and how to address them:
Emotional flooding: If sessions feel too intense, ask your therapist to slow the pace or spend more time on stabilization before targeting memories.
Avoidance: It's natural to want to skip sessions when things feel hard. Name it with your therapist. Avoidance often signals that an important memory is close to the surface.
Skepticism about EMDR: Some people feel uncertain about the eye movement component. That's okay. Talk to your therapist about the research, and remember that the relationship and safety you feel matter as much as the technique.
Needing to change therapists: If you don't feel safe or understood after several sessions, it's appropriate to seek a better fit. Therapeutic alliance is one of the strongest predictors of outcome.
Comorbid anxiety or depression: Research shows no significant difference in PTSD recovery between EMDR and trauma-focused CBT, though tfCBT may reduce comorbid anxiety and depression more effectively when those symptoms are elevated at the start.
Remember: Every small step counts. Showing up to a session when you didn't want to is progress. Naming a feeling you used to suppress is progress. Healing doesn't always look dramatic.
The trauma healing process workflow offers a visual map of these stages that can help you see where you are and what comes next. If you're unsure whether your current approach is the right fit, trauma assessment guidance can help clarify next steps.
Verifying progress and sustaining long-term recovery
Progress in trauma therapy isn't always obvious in the moment. You might not notice change until you realize you handled a situation differently, or that a memory no longer hijacks your day. Tracking your healing intentionally helps you see how far you've come.
Key milestones to watch for:
| Milestone | What it looks like |
|---|---|
| Reduced reactivity | Triggers feel less intense or shorter in duration |
| Better sleep | Fewer nightmares, more restful nights |
| Increased presence | Feeling more grounded in daily life |
| Shifting beliefs | Replacing self-blame with self-compassion |
| Improved relationships | More capacity for trust and connection |
Research supports real, measurable outcomes. Reliable improvement is seen in 60 to 80% of people who complete EMDR treatment in research settings. That's not a small number.
Strategies for sustaining your gains:
Continue using grounding and self-regulation tools even when you feel well
Schedule periodic check-ins with your therapist, even after formal treatment ends
Build community, whether through support groups, trusted relationships, or culturally affirming spaces
Know your early warning signs and have a plan for returning to therapy if needed
For more on what lasting recovery looks like in practice, lasting change with EMDR offers real-world perspective. And if you want to explore specific techniques used in sessions, EMDR intervention examples breaks them down clearly.
A new perspective: Why your trauma healing journey is unique and what truly works
Here's something the research debates often miss: the best therapy isn't the one with the highest average recovery rate. It's the one that fits you, your culture, your pace, your history, and your readiness.
The EMDR versus tfCBT conversation is useful for clinicians, but for you, it can become a distraction. What matters more is whether you feel safe with your therapist, whether the approach respects your identity, and whether you have room to move at your own speed. We've seen clients make remarkable progress with EMDR after years of feeling stuck, and we've seen others need more stabilization time before any memory processing could begin. Neither path is wrong.
Self-compassion isn't a soft add-on to evidence-based care. It's part of what makes healing stick. Trauma often leaves people with deep shame and self-criticism. Therapy that challenges those beliefs directly, while also offering practical tools, tends to produce the most durable change.
Blending structured healing steps with lived experience and community support is what the blending healing strategies framework is built on. Therapy is a tool, not a test. Progress is always possible, even when it's slow.
Ready for support? Trauma therapy resources in California
Reading about healing is a meaningful first step. But at some point, information becomes most powerful when paired with real support.
At Alvarado Therapy, we offer trauma-informed therapy and EMDR sessions for adults across California, including those healing from PTSD and complex trauma. Our licensed therapists work in English and Spanish, and we serve clients in Pasadena, Ventura, and online throughout the state. Whether you're just beginning to explore therapy or ready to start EMDR, we're here to help you take that next step. Request a consultation today and find out what trauma-informed care can look like for you.
Frequently asked questions
What is the first step in trauma healing with EMDR?
You start with building a sense of safety and learning coping skills before moving on to processing traumatic memories. The APA's 2025 PTSD guidelines support this stabilization-first approach as part of EMDR treatment for adults.
How long does it take to see progress in trauma therapy?
Many people notice real improvements within several weeks or months, though the timeline depends on the type and severity of trauma. Studies show reliable improvement in 60 to 80% of people who complete EMDR treatment.
Can I combine EMDR with other therapies?
Yes, EMDR can be used alongside trauma-focused CBT or other evidence-based approaches. Research shows no significant difference in PTSD outcomes between the two, and combining methods can address different symptoms more fully.
Is trauma healing different for childhood trauma or PTSD?
The core steps are similar, but childhood trauma often requires more time in the stabilization phase and extra attention to trust and safety. Trauma-informed principles like empowerment and collaboration are especially important when early experiences involved a loss of control.