What is trauma informed care: a 2026 guide for healing
Trauma-informed care is more than a therapy technique. It's a comprehensive framework that transforms how healing happens. With approximately 60% of adults experiencing at least one traumatic event in their lifetime, understanding this approach is essential. This guide explores trauma-informed care's core principles, how EMDR therapy fits in, and why culturally responsive bilingual services matter for effective healing in California.
Table of Contents
Understanding Trauma-Informed Care: Definition And Importance
EMDR Therapy In Trauma-Informed Care: A Synergistic Approach
Cultural Responsiveness And Bilingual Services In Trauma-Informed Care
How To Find And Prepare For Trauma-Informed Therapy In California
Explore Trauma-Informed EMDR Therapy Services At Alvarado Therapy
Key takeaways
| Point | Details |
|---|---|
| Trauma-informed care framework | Centers on safety, trust, empowerment, and cultural sensitivity rather than being a single therapy method. |
| EMDR therapy integration | Complements trauma-informed care with evidence-based reprocessing that empowers clients to heal at their own pace. |
| Cultural responsiveness matters | Bilingual and culturally sensitive services significantly improve engagement, retention, and healing outcomes in California. |
| Common misconceptions | Many people mistakenly view trauma-informed care as rushed treatment or just another technique when it’s actually a holistic framework. |
| Finding the right therapist | Verify trauma training, EMDR expertise, cultural competence, and commitment to client empowerment before starting therapy. |
Understanding trauma-informed care: definition and importance
Trauma-informed care is a framework that acknowledges trauma's widespread impact and focuses on creating safety and empowerment in treatment environments. It's not a specific therapy type. Instead, it guides how all services are delivered to trauma survivors.
Trauma affects most adults at some point. Research shows about 60% experience traumatic events during their lives. These experiences profoundly shape how people view themselves, relationships, and safety. Traditional mental health approaches often missed this context, focusing only on symptoms.
The shift from "What's wrong with you?" to "What happened to you?" defines trauma-informed care. This reframe recognizes that behaviors labeled as problems are often survival strategies. A person who seems resistant to connection may be protecting themselves based on past betrayals. Someone with anxiety might be responding to real threats they've faced.
Trauma-informed care applies beyond therapy offices. Schools, hospitals, social services, and workplaces benefit from this approach. Any environment where trauma survivors receive support gains from understanding trauma's effects.
Key benefits of trauma-informed care include:
Creating physical and emotional safety that allows healing to begin
Reducing retraumatization through thoughtful policies and practices
Empowering clients to participate actively in their own recovery
Building trust through transparency and consistent boundaries
Recognizing cultural contexts that shape trauma experiences and healing paths
The SAMHSA trauma-informed care framework provides detailed guidance for organizations implementing these principles across different settings.
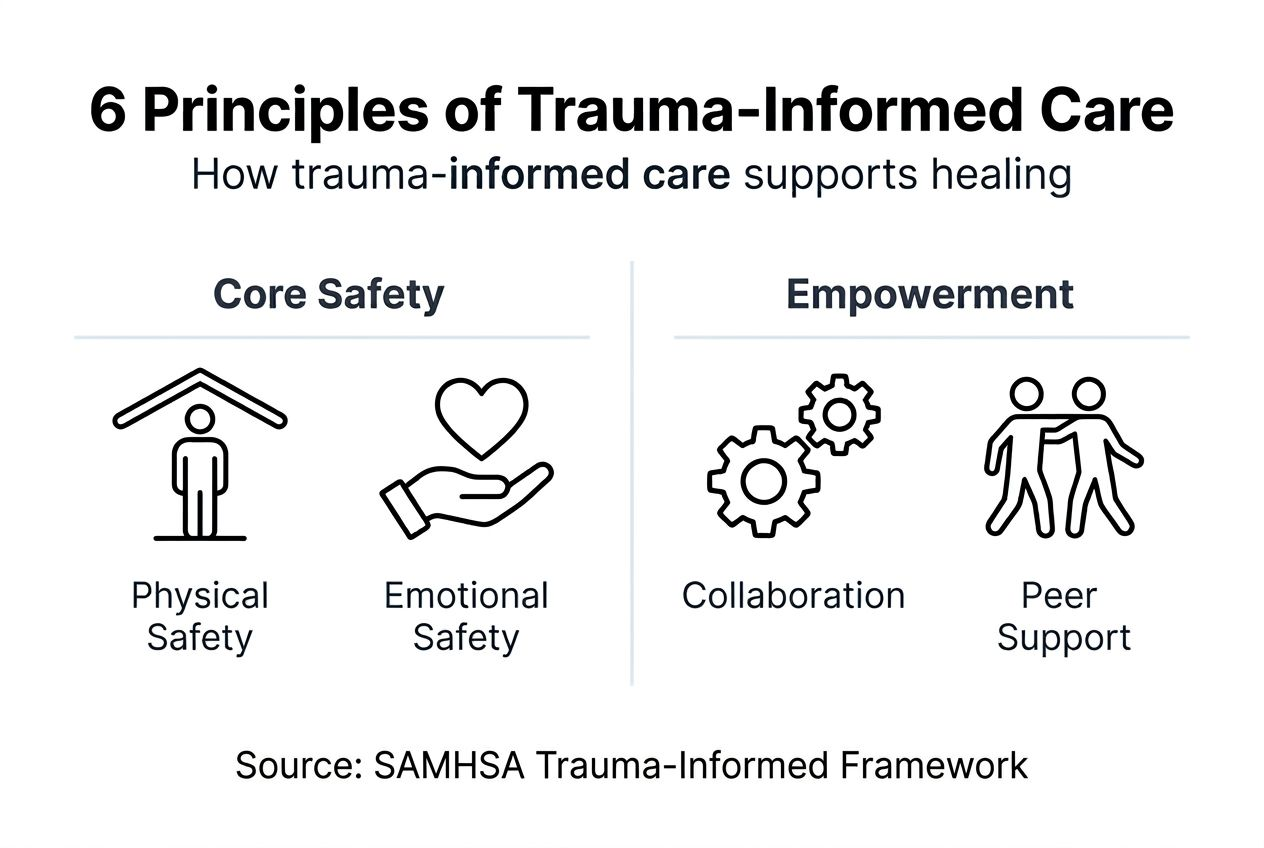
Core principles of trauma-informed care
Trauma-informed care operates on six key principles: safety, trustworthiness, peer support, collaboration, empowerment, and cultural responsiveness. These aren't just ideals. They're practical guidelines that shape every interaction.
Safety comes first, both physical and emotional. Treatment spaces must feel secure. Providers explain procedures before starting them. Clients know what to expect. Emotional safety means avoiding shame, judgment, or pressure. When people feel safe, they can focus on healing instead of protecting themselves.
Trustworthiness and transparency build the foundation for therapeutic relationships. Providers are clear about their qualifications, treatment approaches, and limitations. They keep commitments and maintain consistent boundaries. When trust breaks, they acknowledge it and work to repair the rupture.
Peer support connects trauma survivors with others who understand their experiences. Shared stories reduce isolation and shame. Seeing others heal inspires hope. Many trauma-informed programs include peer specialists who've navigated similar journeys.
Collaboration means why trauma informed care empowers healing by treating clients as partners rather than passive recipients. Providers share power in decision-making. They respect client expertise about their own lives. Treatment plans reflect client goals, not just professional opinions.
Empowerment focuses on strengths and resilience. Providers help clients recognize skills they've developed through surviving trauma. They support clients in building new capacities. The goal is restoring a sense of control that trauma often steals.
Cultural responsiveness acknowledges that culture shapes trauma experiences and healing. Providers examine their own biases. They adapt approaches to honor diverse backgrounds. Language access, cultural traditions, and identity-affirming care become priorities.
Pro Tip: Ask potential therapists how they implement these six principles in their practice. Strong answers include specific examples rather than vague assurances. Listen for whether they prioritize your comfort, choices, and cultural needs.
The Restore Mental Health trauma-informed principles guide offers deeper exploration of how these elements work together to create healing environments.
How trauma-informed care differs from traditional therapy
Traditional therapy often starts with diagnosis and symptom reduction. The focus is identifying what's wrong and fixing it. Trauma-informed care starts differently, recognizing that many symptoms seen in trauma survivors are adaptive survival strategies rather than pathology.
Someone with hypervigilance isn't broken. They developed heightened awareness to stay safe in dangerous situations. That skill served them well. Now it might cause exhaustion, but it's not a defect. Traditional approaches might label this as generalized anxiety disorder and prescribe medication. Trauma-informed care asks what threats this person faced and helps them feel safe enough to relax that vigilance.
Retraumatization is a critical concern. Trauma-informed care reduces retraumatization by modifying policies to eliminate restraint and seclusion except as last resorts. Traditional settings might use these interventions more freely, potentially triggering trauma survivors who've experienced coercion or violence.
Client pacing matters deeply in trauma-informed approaches. Survivors control how quickly they explore painful memories. They can pause or slow down when overwhelmed. Traditional therapy sometimes pushes through discomfort, assuming that's necessary for progress. Trauma-informed care trusts that healing happens when people feel safe enough to face their experiences.
| Aspect | Traditional Therapy | Trauma-Informed Care |
|---|---|---|
| Focus | Symptoms and diagnosis | Person and their history |
| Client role | Passive recipient | Active partner |
| Pacing | Provider-directed | Client-controlled |
| Symptoms | Problems to eliminate | Survival strategies to understand |
| Power | Provider as expert | Shared expertise and decision-making |
Benefits of trauma-informed care over traditional approaches include:
Lower dropout rates as clients feel more respected and understood
Reduced retraumatization during treatment itself
Greater client engagement and motivation
Better long-term outcomes through empowerment focus
Stronger therapeutic alliances built on trust and collaboration
Pro Tip: In your first session, notice whether your therapist asks about your trauma history with sensitivity or rushes through intake forms. Strong trauma-informed therapists let you share at your own pace and explain how they'll use information to support you.
Learn more about differences in trauma care approach and review SAMHSA trauma care retraumatization data to understand why these distinctions matter for your healing journey.
EMDR therapy in trauma-informed care: a synergistic approach
EMDR therapy is recognizedas an effective evidence-based treatment for PTSD and complex trauma, with benefits extending to anxiety and depression. Eye Movement Desensitization and Reprocessing helps your brain process traumatic memories that got stuck. These memories stay vivid and distressing because they weren't fully processed when they happened.
EMDR uses bilateral stimulation, typically eye movements, to activate both brain hemispheres while you recall traumatic events. This mimics what happens naturally during REM sleep when your brain processes experiences. The result is that memories lose their emotional charge. You still remember what happened, but it no longer triggers the same intense reactions.
Typical EMDR therapy process includes these steps:
History taking and treatment planning to identify trauma targets
Preparation phase building coping skills and establishing safety
Assessment of specific memories to process, including negative beliefs they created
Desensitization using bilateral stimulation while focusing on trauma memories
Installation of positive beliefs to replace negative ones
Body scan to identify and release any remaining physical tension
Closure ensuring you feel stable before leaving each session
Reevaluation checking progress and identifying any remaining issues
EMDR aligns perfectly with trauma-informed principles. It empowers clients by letting them control the pace. You decide which memories to address and when to pause. The therapist guides the process but doesn't direct the content of your thoughts. This preserves your autonomy throughout healing.
Safety is built into EMDR structure. The preparation phase ensures you have skills to manage distress. You can stop processing anytime. Therapists check in frequently about your comfort level. This prevents overwhelm and retraumatization.
Benefits of EMDR in trauma care include:
Faster processing than traditional talk therapy for many people
Less need to describe traumatic details verbally, which can feel retraumatizing
Physiological release of trauma stored in the body
Reduced avoidance as memories become less threatening
Improved self-concept as negative beliefs shift
Explore EMDR intensives for trauma healing to learn about accelerated formats. Review Harvard Health EMDR evidence for research supporting this approach.
Cultural responsiveness and bilingual services in trauma-informed care
Cultural identity profoundly affects trauma experiences and healing paths. What feels safe, how emotions are expressed, and what recovery looks like varies across cultures. Trauma-informed care must honor these differences to be truly effective.
Bilingual services significantly improve therapy engagement and outcomes. Speaking your first language in therapy allows deeper emotional expression. Nuances and cultural concepts translate poorly. When you struggle to find English words for complex feelings, therapy becomes harder. Bilingual therapists eliminate this barrier.
Research shows better retention rates with culturally matched therapists. Clients stay in treatment longer when they feel understood not just clinically but culturally. They're more likely to complete therapy and maintain gains afterward.
Advantages of culturally responsive trauma care include:
Reduced shame for clients whose cultures stigmatize mental health treatment
Better understanding of family dynamics and cultural expectations affecting recovery
Appropriate interventions that respect cultural values and traditions
Recognition of collective trauma affecting entire communities, not just individuals
Validation of cultural strengths and resilience practices
California's diversity demands this cultural competence. Immigration trauma, discrimination, and cultural displacement affect many residents. Standard approaches developed for different populations may miss crucial context. Culturally responsive therapy benefits become clear when clients can bring their whole selves to treatment.
Barriers to culturally sensitive care include provider shortage, lack of cultural training, and systemic biases. Many therapists receive minimal education about working across cultures. Insurance networks may not include diverse providers. These gaps leave trauma survivors without appropriate support.
The role of bilingual therapists in trauma recovery extends beyond translation. It includes understanding cultural trauma responses, family structures, and community healing practices. When you find culturally sensitive therapists in CA, you access care that truly fits your needs and honors your identity.
Common misconceptions about trauma-informed care
Many people misunderstand trauma-informed care, which can prevent them from seeking help or recognizing quality treatment. Trauma-informed care is a broad framework guiding service delivery, not a single therapy method. This distinction matters because clients sometimes expect a specific technique when they request trauma-informed care.
Another misconception is that trauma symptoms indicate personal weakness or mental illness requiring medication alone. Actually, symptoms like hypervigilance, emotional numbing, or relationship difficulties often represent adaptive responses to real threats. These strategies helped you survive. They're not character flaws.
Some believe trauma healing must happen quickly or follow a set timeline. Trauma-informed care rejects this idea. Healing is not linear. You might progress, plateau, or temporarily struggle more as deeper issues surface. Providers who push rapid recovery or impose their timeline are not truly trauma-informed.
Top misconceptions about trauma-informed care:
It's a specific therapy technique you can learn in one session
Only people with PTSD diagnoses need trauma-informed approaches
Trauma-informed care means never feeling uncomfortable in therapy
All therapists who mention trauma are equally trained in trauma-informed practices
Realistic expectations help you engage more effectively with treatment. Trauma-informed care creates safety and empowerment, but healing still requires facing painful experiences. The difference is you control the process and receive support throughout.
Clients sometimes expect that trauma-informed therapists will never challenge them. Actually, good trauma-informed care includes gentle challenges when you're ready. The key is how challenges are offered with respect for your autonomy and timing, never through coercion or shame.
Review Restore Mental Health trauma misconceptions to deepen your understanding and approach treatment with clarity about what to expect and what quality care looks like.
How to find and prepare for trauma-informed therapy in California
Choosing a trauma-informed therapist requires verifying specific qualifications and approaches. Look for training in trauma treatment, EMDR or other evidence-based trauma therapies, and cultural competence. Bilingual capacity matters if you prefer therapy in your first language.
Steps to find and select your trauma-informed provider:
Research therapists specializing in trauma in your California area
Check credentials including trauma-specific training and certifications
Review therapist profiles for mentions of EMDR, cultural responsiveness, and bilingual services
Schedule consultations with 2 to 3 therapists to compare approaches
Ask specific questions about their trauma-informed practices
Notice how comfortable and respected you feel during the consultation
Make your choice based on expertise, fit, and your gut feeling about safety
Trauma Informed California offersmulti-day training programs providing continuing education credits to raise practitioner competency. Therapists with this certification demonstrate commitment to trauma-informed principles.
Questions to ask prospective therapists:
What specific training have you completed in trauma treatment and EMDR?
How do you create safety and avoid retraumatization in your practice?
Can you describe your approach to client empowerment and collaboration?
What experience do you have working with my cultural background?
How do you handle situations when I need to slow down or pause processing?
What happens if I don't feel ready to discuss certain traumatic memories?
Strong answers include specific examples, acknowledgment of your concerns, and clear explanations of their process. Vague responses or defensiveness are red flags. Trust your instincts about whether this person feels safe.
Pro Tip: Before starting therapy, identify 2 to 3 coping skills that help you feel grounded. Practice them regularly. Having these tools ready makes the preparation phase of EMDR and other trauma work more effective. Your therapist can build on skills you've already developed.
Verify cultural competence by asking about the therapist's experience with your specific background and any additional training they've pursued. Generic statements about valuing diversity matter less than concrete examples of culturally adapted interventions.
Learn how to prepare for counseling as a trauma survivor and review this 7-step checklist for starting trauma therapy to maximize your chances of successful healing. Explore Trauma Informed California training to understand what quality trauma education includes.
Explore trauma-informed EMDR therapy services at Alvarado Therapy
Alvarado Therapy offers specialized trauma-informed care with EMDR therapy at its core. Licensed therapists across Pasadena, Ventura, and online throughout California provide bilingual services in English and Spanish. This ensures you receive care in your preferred language with culturally responsive approaches.
Discover online EMDR trauma therapy that brings healing to your home with convenience and privacy. The team specializes in PTSD and complex trauma services including EMDR intensives for accelerated processing. These concentrated formats help you make significant progress in days rather than months.
Schedule therapy consultations to discuss your specific needs and goals. Alvarado therapists understand immigration trauma, childhood experiences, and the unique challenges California's diverse communities face. They'll help you create a personalized healing plan that honors your pace, culture, and vision for recovery. Access to trauma-informed care is just a consultation away.
FAQ
What is trauma-informed care?
Trauma-informed care is a framework that recognizes trauma's widespread impact and emphasizes safety, trust, and empowerment in treatment. It shifts focus from symptoms to understanding how past experiences shape current behaviors. This approach applies across all service settings, not just therapy, creating environments where trauma survivors can heal without retraumatization.
How does EMDR therapy help with trauma?
EMDR therapy helps your brain reprocess traumatic memories that remain distressing because they weren't fully processed when they occurred. Using bilateral stimulation like eye movements, EMDR reduces the emotional charge of these memories. You remember what happened but without the intense reactions, allowing you to move forward with less fear and more peace.
Why are bilingual trauma-informed services important in California?
Bilingual services allow deeper emotional expression in your first language, where nuances and cultural concepts translate more authentically. Language access improves therapy engagement, retention, and outcomes. California's diverse population includes many who prefer or need services in languages other than English. Cultural responsiveness combined with language access ensures truly effective trauma healing that honors your whole identity.
What should I ask a therapist to ensure they are trauma-informed?
Ask about specific trauma training, EMDR or other evidence-based trauma therapy experience, and their approach to creating safety and client empowerment. Inquire how they handle situations when you need to slow down processing and their experience with your cultural background. Strong therapists provide concrete examples rather than vague assurances. Listen for whether they prioritize your autonomy, comfort, and cultural needs in their answers.
Can trauma-informed care prevent retraumatization during therapy?
Trauma-informed care significantly reduces retraumatization through client-controlled pacing, thoughtful policies, and emphasis on safety. Therapists avoid coercive interventions, explain procedures before implementing them, and respect your boundaries. While healing sometimes involves discomfort as you face painful memories, trauma-informed approaches ensure you maintain control throughout the process and receive support when distress arises.